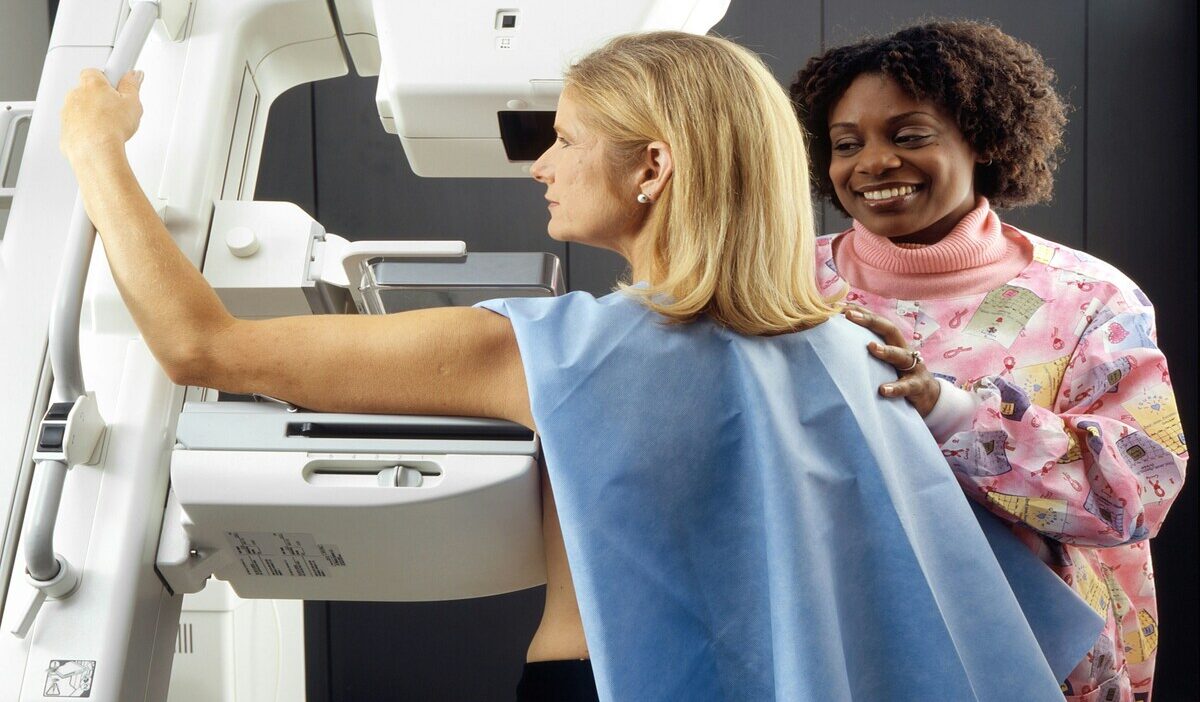
Breast cancer screening is one of the most important preventive health services for older adults. As people approach retirement age, many begin asking a simple but critical question: Does Medicare cover mammograms?
In this guide, we’ll explain does Medicare cover mammograms, how often coverage applies, what costs you might expect, and how screening mammograms differ from diagnostic ones.
1. Does Medicare Cover Mammograms?
The short answer is yes. Medicare does cover mammograms for eligible beneficiaries.
Medicare Part B covers mammograms as a preventive service used to detect breast cancer early. Specifically, Medicare typically covers:
- One baseline mammogram between ages 35 and 39
- One screening mammogram every 12 months for women age 40 and older
- Diagnostic mammograms when medically necessary
This means that for most beneficiaries, the answer to does Medicare cover mammograms is yes, especially for routine breast cancer screening.
Another important detail is cost. Medicare generally covers screening mammograms at 100% of the Medicare-approved amount, meaning patients often pay nothing if the provider accepts Medicare assignment.
Because breast cancer risk increases with age, these preventive screenings remain an essential benefit for Medicare patients.
2. How Often Does Medicare Pay for Mammograms?
When people ask does Medicare cover mammograms, they are usually also wondering how frequently Medicare will pay for them. Fortunately, Medicare has clear rules regarding how often screening or diagnostic tests can be covered.
>>> Read more: How to Get a Free iPhone: Legit Ways to Get an iPhone at No Cost
Annual screening mammograms
Screening mammograms are routine breast cancer screenings for individuals who do not have symptoms. For most beneficiaries, Medicare Part B covers one screening mammogram every 12 months for women age 40 or older.
Because Medicare treats these screenings as preventive care, patients typically pay nothing for the exam if the healthcare provider accepts Medicare assignment.
This policy is why many people researching does Medicare cover mammograms learn that the program strongly supports annual preventive screenings.
Early detection is critical. According to research and public health guidelines, regular mammograms can identify breast cancer before physical symptoms appear, allowing treatment to begin sooner.
Diagnostic mammograms
A diagnostic mammogram is different from a screening mammogram. Instead of routine preventive screening, it is ordered when a doctor needs to investigate a specific concern, such as a lump, pain, or abnormal screening result.
Medicare still covers diagnostic mammograms, but the cost rules differ slightly. Beneficiaries usually must first meet the Part B deductible, and then they pay 20% of the Medicare-approved amount for the service.
Unlike screening tests, diagnostic mammograms are not limited to once per year. If your doctor determines that additional imaging is medically necessary, Medicare may cover multiple diagnostic mammograms in the same year.
This is another reason why the question does Medicare cover mammograms often depends on the type of mammogram ordered.
Does Medicare cover mammograms after age 65?
Many beneficiaries wonder does Medicare cover mammograms after age 65. The answer is yes.
In fact, most people first become eligible for Medicare at age 65, so breast cancer screening remains a common preventive service among Medicare patients.
Medicare continues to cover annual screening mammograms for women age 40 and older, including those who are over 65. There is no automatic age cutoff for this preventive service.
Because the risk of breast cancer increases with age, doctors often recommend continued screening for older adults who are in good health.
Therefore, when patients ask does Medicare cover mammograms after age 65, the answer remains the same: Medicare continues to provide coverage for routine screenings.
Does Medicare cover yearly mammograms after age 75?
Medicare itself does not impose a strict upper age limit for mammogram coverage. As long as a patient remains enrolled in Medicare Part B and the screening is medically appropriate, Medicare can still cover yearly mammograms.
However, doctors sometimes adjust screening recommendations based on overall health and life expectancy. Some medical guidelines suggest that screening decisions after age 75 should be individualized based on the patient’s health status and preferences.
Still, for many beneficiaries, the answer to does Medicare cover mammograms remains yes even after age 75.
3. Screening vs Diagnostic Mammograms: What’s the Difference?
Understanding the difference between screening and diagnostic tests helps clarify does Medicare cover mammograms and how costs may vary.
A screening mammogram is a preventive test performed when there are no symptoms or signs of breast disease. The goal is to detect cancer early, often before it can be felt during a physical exam.
A diagnostic mammogram, on the other hand, is performed when a doctor needs more detailed imaging. This may happen if a screening test shows an abnormal area or if the patient experiences symptoms such as breast pain, a lump, or unusual discharge.
Medicare treats these two services differently. Screening mammograms are considered preventive care and are typically covered with no out-of-pocket cost when providers accept Medicare assignment.
Diagnostic mammograms, however, fall under standard Part B coverage rules, which may require coinsurance.
Because of these differences, understanding the type of exam ordered by your doctor is important when asking does Medicare cover mammograms.
>>> Read more: How to Get a Free iPhone 11: Legit Ways to Qualify in 2026
4. What Costs Might Medicare Patients Pay?
Although Medicare provides strong preventive coverage, some patients may still encounter costs depending on the type of mammogram performed.
For routine screening mammograms, Medicare typically covers the entire cost if the provider accepts Medicare assignment. Patients usually pay nothing for the screening itself.
Costs may apply in certain situations, however. If the mammogram is diagnostic rather than preventive, Medicare beneficiaries generally must pay the Part B deductible and then cover 20% of the approved amount.
Additional costs may also occur if:
- The provider does not accept Medicare assignment
- Additional imaging tests are required
- The patient receives services outside their Medicare Advantage network
Understanding these details can help beneficiaries better interpret the answer to does Medicare cover mammograms and avoid unexpected medical bills.
Conclusion
For most beneficiaries, the answer to does Medicare cover mammograms is reassuring. Medicare Part B includes mammograms as a preventive service designed to detect breast cancer early and improve health outcomes.
The program generally covers one screening mammogram every 12 months for women age 40 and older, with no out-of-pocket cost when the provider accepts Medicare assignment. Diagnostic mammograms are also covered when medically necessary, although they may involve deductibles or coinsurance.